1990s
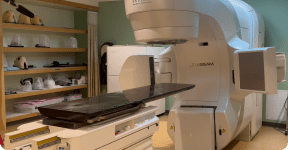
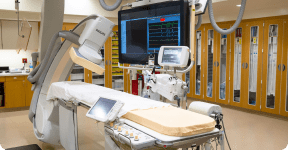
The 1990s were a period of significant progress for Bay Area Hospital. Highlights included the construction of the Radiation Therapy Center in 1990 and investments in new technologies, such as an integrated computer system, in 1991. In 1997, a state-of-the-art CT scanner was installed, and by 1998, mammography and stereotactic breast biopsy services were introduced, alongside the opening of a $1 million angiography suite. The hospital underwent further transformation in 1999, with the remodeling of the psychiatric services facility, the introduction of new access roads, and the unveiling of its first website.